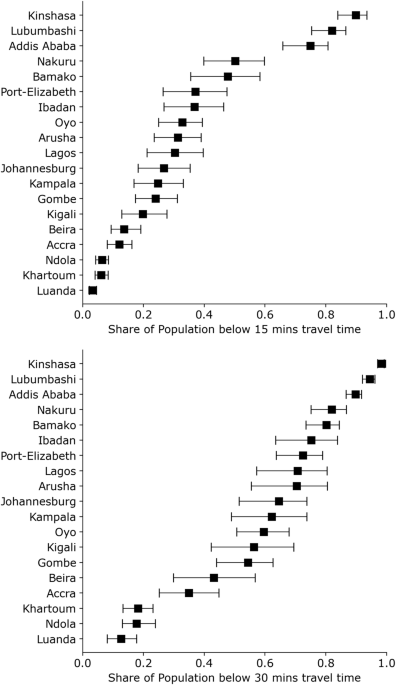
Our analysis reveals significant differences in spatial accessibility (SA) to healthcare facilities across various sub-Saharan African (SSA) cities, underscoring the intricate relationship between urban planning, land use, and health equity. The disparities in SA between formal and informal areas within these cities highlight the ongoing challenges in urban health provisioning, particularly in rapidly expanding urban environments. These findings are critical as they emphasize the uneven distribution of healthcare resources, which can have profound implications on public health outcomes, especially for vulnerable populations residing in informal settlements.
While ref. 3 found that 39.8 and 56.9% of the global population can reach healthcare by foot within 30 and 60 min, respectively, we show that the values for urban populations are higher. We find that 58 and 78% of the urban population in the SSA cities surveyed can reach a health facility within 30 and 60 min. Nevertheless, we found that the values differ when a distinction between formal and informal areas is made. For example, 63.2% of the population living in formal areas has travel times below 30 min, while only 55.4% of the population in informal areas meets this threshold. This disparity not only reflects the historical neglect of informal settlements in urban planning but also poses a significant public health risk, as these populations may be more vulnerable to outbreaks of disease and other health crises.
Based on previous analyses, we were also able to calculate the relative risk of having access below a certain travel time for the cities considered in this study. We found that in some of the cities (Addis Ababa, Beira, Khartoum, and Ndola), living in an informal area is a risk factor for having limited access to healthcare facilities. Since the relative risk is independent of the SA and the size of the respective city, further work is required to understand the implications of these findings.
Interestingly, our analysis (cf. Fig. 4) confirmed the importance of medium-sized cities, as mentioned in other publications such as the World Cities Report10 or the sixth report of the IPCC36. Both publications highlight the importance of these areas, often referred to as secondary cities, due to their high growth rates in area and population. We emphasize their particular importance by finding that, especially in these cities, populations living in informal areas are disadvantaged in their access to healthcare.
The travel time maps and the heterogeneity of spatial accessibility (SA) to health infrastructures within informal areas highlight the diverse living conditions for inhabitants, even with similar morphology serving as the basis for area identification. Our results, derived from satellite imagery, underscore the variability in living conditions within these settlements. This emphasizes the significance of comprehensive analysis, as advocated by global initiatives like IDEAMaps9, to effectively implement suitable upgrading concepts. Assuming that the dataset provided by ref. 24 is accurate, these maps provide valuable information on the locations within the city where healthcare infrastructure is necessary.
In our study, we analyzed accessibility to healthcare facilities specifically by walking, whereas ref. 16 assessed accessibility to comprehensive emergency obstetric care facilities across 15 Nigerian cities using travel time estimates from Google Maps, which primarily include driving as the mode of transportation. This methodological difference allows for a meaningful comparison between the two approaches in the context of Lagos and Ibadan.
For Ibadan, ref. 16 reported spatial accessibility (SA) of 44.9% within 15 min and 79.8% within 30 min when considering only public facilities. In contrast, our study, which focuses solely on hospitals (Group (i)) and considers walking as the mode of travel, found significantly lower SA values of 2.9% for 15 min and 12.6% for 30 min. Similarly, in Lagos, they found SA values of 45.8% for 15 min and 83.7% for 30 min, while our study found 4% (15 min) and 15.9% (30 min).
These stark differences in SA percentages can be primarily attributed to the mode of transportation considered in each study. By focusing on walking, our approach is inherently more conservative and is designed to detect population groups with insufficient access to healthcare under more constrained mobility conditions. In contrast, ref. 16 use of driving times likely reflects faster travel times and greater accessibility in urban areas. Although the number of hospitals considered was similar between the two studies, the choice of transportation mode plays a crucial role in accessibility outcomes. Therefore, while both sets of results are reasonable within their respective contexts, our conservative approach highlights potential disparities in healthcare access that might be overlooked when considering faster modes of transportation.
With our results, we are also able to compare intra-urban SA with national SA to hospitals (Group (i)) in SSA (cf. Table 3). We observe various patterns. For the cities of Accra, Beira, and Nakuru, we observe that the citywide percentage of the population outside 2-h travel time is above the national values. Nevertheless, while in all of these cities, the percentage of the population outside a 2-hour travel time living in formal areas is below the national average, the value for informal areas is higher. This indicates that the population in informal areas is disadvantaged not only in comparison to formal areas within the city but also in comparison to the city as a whole. These findings are supported by the relative risks presented in Table S1 in Supplementary Information, where seven cities show an increased risk for individuals in informal areas of having worse access to hospitals within 120 min than those living in formal areas.
In contrast, we also identified several cities where national values are considerably higher than citywide formal and informal SA values (Addis Ababa, Arusha, Bamako, Khartoum, Kinshasa, Luanda, Lubumbashi, and Oyo). All of these cities confirm the often observed finding that large cities are often advantaged in comparison to other parts of the country in terms of accessibility to healthcare3. Lastly, we find that in Johannesburg and Port Elizabeth, the national value for South Africa is considerably lower than the citywide, informal, and formal values. Given that South Africa is reported to have higher SA to healthcare compared to other SSA cities, this finding needs further investigation and could be influenced by the data used to conduct our study and its associated limitations.
The relevance of this study extends beyond the immediate findings on spatial accessibility (SA) to healthcare facilities in Sub-Saharan African (SSA) cities. The disparities highlighted between formal and informal urban settlements underscore broader issues of inequality that are crucial to urban planning and public health. In rapidly urbanizing regions, where informal settlements continue to expand, ensuring equitable access to essential services like healthcare is a pressing challenge. These findings underscore the need for urban planners and policymakers to prioritize the inclusion of informal areas in urban development plans, particularly in healthcare provisioning.
Urban planning often prioritizes formal areas due to their regulated nature and easier integration into city-wide infrastructure networks. However, as this study demonstrates, neglecting informal settlements can exacerbate existing health inequities, leaving large segments of the urban population vulnerable to disease outbreaks and other health crises. The study’s findings serve as a critical reminder that achieving health equity in urban settings requires an inclusive approach that addresses the needs of all urban residents, regardless of the formal status of their living conditions37.
The disparities in healthcare accessibility revealed by this study have profound implications for public health outcomes in SSA cities. Limited access to healthcare facilities in informal settlements not only increases the risk of untreated illnesses but also contributes to broader public health challenges, such as the spread of infectious diseases. The relative risk analysis indicating that residents of informal settlements are more likely to experience limited access to healthcare reinforces the urgent need for targeted public health interventions in these areas.
To work as consistently as possible, we used globally or continentally available products such as the healthcare dataset from ref. 24, the WorldPop data25 for gridded population maps, land use data23 to distinguish between formal and informal areas, and OpenStreetMap to calculate travel times. All of these products introduce various types of uncertainties into our analysis.
It is acknowledged that gridded population datasets, such as the WorldPop dataset utilized in this analysis, exhibit considerable uncertainty when estimating the number of individuals residing in slums. A comparison of gridded population estimates with demographic health survey data31 or other data from the literature32 in different cities in the Global South indicates that the number of individuals residing in informal areas may be ten times higher than suggested by the estimates. In comparing local survey data with gridded population datasets, ref. 38 demonstrated that self-reported population numbers are, on average, up to double the size of gridded population estimates. Consequently, the values calculated for spatial accessibility can be considered a lower boundary for the actual values.
We recognize that the potential incompleteness of OSM data could introduce a degree of bias to our findings. However, OSM street network data have been successfully used to replicate land-use parcels39 or improve land cover products40 in several African cities. Moreover, global analyses are quite encouraging and highlight the constant improvement of data quality and completeness41,42. Future studies should consider evaluating road completeness, as was recently done by Herfort43 for building footprints.
The land-use classification we based our analysis on has an accuracy of 71%23, leaving room for several uncertainties. Nevertheless, the classification of informal areas as such is challenging and a highly debated field. Especially the issue of having adequate ground truth data as well as clearly defining informal settlements from a spatial perspective (What is an informal area, and what is not?) is an open question still under research7,9,20.
Another limitation comes from the dataset on healthcare facilities. Lists of healthcare facilities in sub-Saharan Africa (SSA) are incomplete2. While the data seem reasonable for some of the cities, the number of healthcare facilities in other cities (e.g., Luanda) is considered too low. This clearly affects the results. Moreover, we did not account for localized factors that can affect accessibility, such as informal vendors, lack of maintenance, and irregular surfaces, as this would require data that is beyond the scope and capacity of our current analysis. However, it is recommended that studies at smaller scales attempt to include these factors to increase the accuracy of the results.
Although information on healthcare facilities is also available from other sources, such as OSM or Google Maps, the dataset we used is the only externally evaluated dataset at a continental scale. One limitation of this study is the exclusive focus on public health facilities within the dataset. This approach does not account for the significant role of private healthcare providers, which, for instance, constitute over 45% of all health facilities in Kenya44. It should be noted that the importance of private clinics varies significantly depending on the political and economic context of each country. While this focus on public facilities is a necessary first step in understanding access to healthcare, it may lead to an incomplete picture of the overall healthcare landscape.
Another possible bias in the dataset is that information on healthcare facilities could be outdated (e.g., due to destruction in armed conflicts). Additionally, the capacity of healthcare facilities was omitted from our analysis, limiting our ability to conduct a more nuanced evaluation. Larger facilities with greater capacity typically serve more people, potentially skewing accessibility results if not considered, as they may reduce pressure on smaller, nearby facilities. Conversely, smaller facilities might be overwhelmed, reducing access and increasing wait times, especially in densely populated areas. Incorporating capacity considerations would have enabled a more detailed analysis, such as a two-step floating catchment area approach.
Moreover, the age of the population plays a crucial role, as older populations generally have higher healthcare needs and more frequent service requirements. Areas with older demographics might experience greater strain on local facilities, complicating accessibility further. Future studies should incorporate both facility capacity and population age to enhance the accuracy of healthcare accessibility assessments.
In our analysis, we exclusively examined the aspect of physical accessibility to healthcare facilities. However, it is essential to acknowledge that healthcare accessibility encompasses various dimensions that extend beyond mere geographic proximity. According to ref. 45, relevant dimensions of access are availability, affordability, and acceptability. Notably, the financial aspect plays a pivotal role, as the costs of treatment may vary significantly among different facilities, potentially influencing individuals to forego the closest option. Another crucial aspect is the social and cultural distance between the healthcare system and its users. Moreover, our analysis lacked granularity in terms of distinguishing between the specialized services offered by healthcare facilities, a crucial factor influencing healthcare-seeking behavior.
By focusing solely on walking, our study provides a conservative estimate of healthcare accessibility, which is particularly relevant in lower-income areas with limited transport options. However, this approach may underestimate actual access for those using other modes of transportation, especially over longer distances where walking is less practical.
This limitation highlights the need for future research to incorporate a broader range of transportation modes, offering a more accurate and comprehensive view of healthcare accessibility in urban areas with diverse transport infrastructures. Despite these limitations, our use of global and continental data products marks an important first step toward systematic inter-urban analyses with meaningful outcomes.
The insights gleaned from our study on SA to healthcare facilities in SSA cities set the stage for promising future research avenues. As we consider the global implications of our findings, extending our analytical framework to a global scale emerges as a pivotal step. Such an expansion would not only facilitate cross-continental comparisons but could also unveil overarching patterns and trends in spatial healthcare accessibility. This broader perspective holds the potential to offer valuable insights for shaping global health planning and policy formulation. To ensure the ongoing relevance and accuracy of our insights, a commitment to integrating the latest available data remains imperative. Regular updates to datasets, encompassing healthcare facility locations, population distribution, and land use information, are essential to capture the dynamic nature of urban landscapes.
As we delve deeper into expanding the scope of our analysis, considering various transportation modes beyond walking could be a major improvement. The inclusion of public transportation networks, road infrastructure, and other relevant transportation modes promises a more nuanced understanding of overall healthcare accessibility in diverse urban settings. Recognizing that healthcare accessibility extends beyond mere physical proximity necessitates the integration of multidimensional travel-time estimates in future studies. This includes considerations of socio-economic accessibility, financial factors, and the availability of specialized healthcare services, contributing to a more comprehensive evaluation of healthcare access.
Integrating information on healthcare facility capacity, including size, capabilities, and services offered, is crucial for refining accessibility analysis. Building on the importance of initiatives like IDEAMaps9, future research should adopt a holistic approach, analyzing living conditions, community needs, and infrastructural challenges alongside spatial accessibility. Expanding the analysis to include socio-economic factors like income, education, and employment will provide a more comprehensive understanding of disparities and guide equitable healthcare policies. Additionally, using advanced methodologies, such as two-step catchment area analysis, can offer a more nuanced view of healthcare access. By addressing these factors collectively, future studies can provide actionable insights for policymakers and urban planners, enhancing social inclusion and healthcare delivery effectiveness.
link