The methodology adopted in this study is centered on a multi-layered smart electrical framework that integrates load forecasting, renewable source management, and critical-area power continuity. The core optimization strategies are supported by a detailed set of mathematical models, allowing for accurate representation of dynamic load allocation, AI-based decision systems, and storage control. Equation (1) to (15) describe real-time load behavior, power distribution logic, and intelligent response algorithms necessary for effective hospital energy management. The system design accommodates redundancy planning and scalable microgrid architecture using predictive models trained on operational and weather-related variables.
Load balancing and power distribution
Load balancing and power distribution are critical aspects of electrical design optimization in hospital infrastructure. Effective distribution of electrical loads ensures that the hospital’s electrical system operates efficiently and prevents overloading, which can lead to blackouts, equipment failure, or energy waste. Hospitals, with their large and diverse energy demands (from HVAC systems to medical equipment), require an optimized approach to power distribution to maintain continuous, reliable service.
Effective distribution of electrical load
In hospitals, the electrical load is dynamic and changing based on time of day, hospital operating requirements, and weather conditions outside. Load balancing refers to the activity of ensuring that electrical energy is distributed evenly throughout all circuits and systems in the building. Not only does it ensure that no single part of the system is overloaded, but it also makes the power supply more reliable in general.
For example, when electrical loads from lighting, HVAC, and medical equipment are not properly balanced, one portion of the system can receive excessive energy, while others receive insufficient power. This may result in abnormally high equipment wear, reduce system operational efficiency, and increase the likelihood of system failure. Balancing the load throughout the system will assist hospitals in reducing energy waste and enhancing the reliability of power supply.
Use of automated monitoring systems
For load balancing, hospitals can fit automatic monitoring systems that dynamically redistribute power distribution in real-time. These systems can monitor energy consumption by department (e.g., emergency, inpatient care, diagnostic) and control the power flow to maintain optimal conditions. Automated systems can change the power load based on several factors such as time of day, peak periods of use, and medical device criticality in an effort to offer energy distribution according to the present needs of the hospital.
Such systems take advantage of real-time data from other sensors and meters strategically located throughout the building32. The system continuously keeps track of the power requirements of each zone, such as operating rooms, emergency rooms, or diagnostic equipment, and regulates the power supply to provide stability and prevent overload. These systems reduce the chances of blackouts, improve equipment lifespan, and minimize downtime during operation. Mathematically, load balancing can be described by the equation:
$$\:{L}_{total}=\sum\:_{i=1}^{n}{L}_{i}$$
(1)
where \(\:{L}_{total}\) is total electrical load of the system, \(\:{L}_{i}\) is Load from each individual unit or department (i.e., HVAC, lighting, medical equipment), \(\:n\) is Number of departments or units.
The goal is to distribute \(\:{L}_{total}\:\)in such a way that no single department exceeds its maximum capacity, ensuring that \(\:{L}_{i}\le\:{L}_{max,i}\) for each \(\:i\), where \(\:{L}_{max,i}\) is the maximum allowable load for each unit.
Dynamic load adjustment using automated systems
Dynamic load adjustment relies on algorithms that use real-time monitoring to forecast load peaks in the load and shifting the distribution33. For example, in a hospital setting, the emergency room’s increased energy needs may be at night, whereas for patient wards, the increased energy usage may be during the day due to medical equipment and lighting.
A simple mathematical model to represent this dynamic load adjustment could be:
$$\:L\left(t\right)=\sum\:_{i=1}^{n}{f}_{i}\left(t\right).{L}_{i}$$
(2)
where \(\:L\left(t\right)\) is Total load at time \(\:t\). \(\:{f}_{i}\left(t\right)\:\)is Load adjustment factor based on time of day and real-time power demands (dynamic factor).
By dynamically adjusting the load based on time and operational requirements, the hospital ensures that no unit is overburdened while maintaining optimal power availability.
Integration of smart grid technologies
The integration of Smart Grid Technologies in hospital electrical systems enhances the operational efficiency, reliability, and sustainability of energy management. By implementing IoT-based monitoring systems, AI-driven demand response mechanisms, and predictive maintenance algorithms, hospitals can optimize energy usage, reduce costs, and improve system resilience.
Implementation of IoT-Based monitoring and control systems
IoT-based monitoring systems assist hospitals to collect real-time data from various electrical appliances across the entire facility, such as HVAC units, lighting systems, medical equipment, and energy storage devices. IoT systems enable dynamic control of energy delivery such that every department of the hospital receives optimal power with minimal wastage. IoT sensors constantly provide data pertaining to voltage, current, and temperature to a centralized control system, which utilizes this information to make intelligent power distribution decisions34.
Each electrical device \(\:i\) in the hospital is equipped with an IoT sensor that reports the power demand \(\:{P}_{i}\left(t\right)\) in real-time. The total power consumption across the hospital at any given time\(\:\:t\:\)can be expressed as:
$$\:{P}_{total}\left(t\right)=\sum\:_{i=1}^{n}{P}_{i}\left(t\right)$$
(3)
where \(\:{P}_{total}\left(t\right)\) is the total power demand of the hospital at time \(\:t\), \(\:{P}_{i}\left(t\right)\) is the power demand of device \(\:i\) at time \(\:t\), \(\:n\) is the number of devices in the hospital.
The IoT-based system collects this data and adjusts the power supply dynamically based on real-time usage patterns. For instance, when certain areas (like administrative offices) are under low occupancy, the system can reduce their power supply by sending a control signal \(\:{f}_{i}\left(t\right)\) to the devices:
$$\:{P}_{i}\left(t\right)={f}_{i}\left(t\right).{P}_{i}^{max}$$
(4)
where \(\:{P}_{i}^{max}\)is the maximum power capacity of device \(\:i\), \(\:{f}_{i}\left(t\right)\) is the dynamic adjustment factor that adjusts the device’s power demand based on occupancy and operational needs.
Use of AI-Driven demand response mechanisms for energy efficiency
AI-driven demand response mechanisms enable hospitals to balance energy supply and demand by forecasting energy needs and making automated adjustments in real time. By utilizing machine learning algorithms, hospitals can predict periods of high demand and implement energy-saving strategies to reduce load during peak times. These systems operate by analyzing historical data and environmental and operational variables, including ambient temperature, patient occupancy, and equipment utilization16. The AI algorithm predicts future energy demand \(\:{\widehat{P}}_{total}\left(t+1\right)\) at time \(\:t+1\)based on historical power consumption data \(\:{P}_{total}\left(t\right)\), weather conditions \(\:W\left(t\right)\), and other factors such as patient occupancy \(\:{N}_{occupancy}\left(t\right)\). The predictive model can be represented as:
$$\:{\widehat{P}}_{total}\left(t+1\right)=f({P}_{total}\left(t\right),W\left(t\right),\:{N}_{occupancy}\left(t\right),\theta\:)$$
(5)
where \(\:f(.)\) is the machine learning function that maps historical data and factors to future power demand, \(\:\theta\:\) represents the model parameters learned through training on historical data.
Using this prediction, the hospital’s AI-based energy management system can initiate demand response strategies. For example, the system may temporarily reduce the cooling load by adjusting the HVAC system power consumption, especially during periods of high temperature and patient occupancy. The power reduction \(\:\varDelta\:{P}_{cooling}\:\)during peak hours can be calculated by:
$$\:\varDelta\:{P}_{cooling}=\alpha\:.{P}_{cooling}^{max}$$
(6)
where \(\:\alpha\:\) is the reduction factor determined by the AI system based on forecasted demand, \(\:{P}_{cooling}^{max}\) is the maximum power consumption of the cooling system. The objective is to reduce the total load \(\:{P}_{total}\) during peak periods while still maintaining the required comfort levels for patients.
Enhancing Real-Time fault detection and predictive maintenance
Real-time fault detection and predictive maintenance are crucial for preventing power failures and extending the lifespan of hospital electrical equipment. By continuously monitoring the health of electrical components (e.g., transformers, circuit breakers, generators), hospitals can detect early signs of malfunction or wear. These systems use predictive analytics to forecast potential failures and schedule maintenance before a failure occurs35. Real-time monitoring involves tracking the operational status of devices, including parameters such as temperature \(\:T\left(t\right),\) vibration \(\:V\left(t\right)\) and current \(\:I\left(t\right).\) Anomalies in these parameters indicate potential faults. The fault detection model checks if the system’s parameters \(\:\left\{T\right(t),V(t),I(t\left)\right\}\) exceed predefined thresholds, triggering alerts for maintenance. The fault detection equation can be expressed as:
$$\:F\left(t\right)=\sum\:_{i=1}^{n}1\left({T}_{i}\right(t)>{T}_{i}^{max}\:or\:{V}_{i}\left(t\right)>{V}_{i}^{max}or{I}_{i}\left(t\right)>{I}_{i}^{max})$$
(7)
where \(\:F\left(t\right)\) is the fault detection function at time \(\:t\), \(\:{T}_{i}\left(t\right),\:{V}_{i}\left(t\right),\:{I}_{i}\left(t\right)\) are the temperature, vibration, and current measurements of device \(\:i\).\(\:\:{T}_{i}^{max},\:{V}_{i}^{max},\:{I}_{i}^{max}\)are the maximum acceptable thresholds for these parameters.
If any of the parameters exceed their thresholds, a fault is detected, and predictive maintenance is scheduled. Predictive maintenance uses a regression model that predicts the remaining useful life (RUL) of a device, based on historical data:
$$\:{RUL}_{i}\left(t\right)=g({T}_{i}\left(t\right),\:{V}_{i}\left(t\right),\:{I}_{i}\left(t\right),\:\tau\:)$$
(8)
where \(\:{RUL}_{i}\left(t\right)\) is the remaining useful life of device iii at time \(\:t\), \(\:g\left(.\right)\) Is the predictive model that estimates RUL based on historical data and real-time parameters, \(\:\tau\:\) represents the historical operating conditions. The RUL prediction helps the hospital schedule maintenance before a failure occurs, ensuring the uninterrupted operation of critical systems like operating rooms and imaging devices.
Redundancy planning and emergency backup systems
Redundancy planning and emergency backup systems are critical components of hospital electrical design optimization. Hospitals, being highly sensitive environments that rely on continuous, uninterrupted power, must be equipped with robust systems to handle power failures, ensuring the safety and well-being of patients. Redundant systems and emergency backup strategies help hospitals maintain functionality, even during unexpected power outages, by leveraging advanced uninterruptible power supplies (UPS), backup generators, and automated fault detection36. Table 4 shown the Redundancy Planning and Emergency Backup Systems in Hospitals.
Optimized placement of electrical panels and outlets
The optimized placement of electrical panels and outlets in hospital environments is a critical factor influencing safety, equipment reliability, and clinical workflow efficiency. Improper positioning can cause increased electromagnetic interference (EMI), cable congestion, and operational delays, particularly in high-dependency zones such as ICUs and operating theatres. According to a 2021 report by the U.S. Department of Veterans Affairs, implementing zoned panel placement and color-coded emergency outlets led to a 17% decrease in electrical incidents and a 12% improvement in procedure readiness37. Similarly, a BIM-based simulation study conducted in a Singaporean tertiary hospital revealed that optimized outlet design reduced nursing path inefficiencies by 15%, lowered cable overlap by 28%, and minimized EMI-related diagnostic faults by up to 9%. Compliance with standards such as NFPA 99, IEC 60364-7-710, and IEEE 1100 is essential to ensure correct spatial clearances, circuit segregation, and fail-safe grounding. Moreover, outlets positioned at ergonomic heights (typically 0.9–1.2 m above floor level) and integrated within modular bedhead trunking systems can improve accessibility while reducing physical strain for healthcare staff. To future-proof infrastructure, outlet locations should also accommodate IoT-enabled power monitoring systems and intelligent switching components to support predictive maintenance. Table 5 summarizes optimal electrical design parameters for different hospital zones based on international benchmarks and clinical performance studies.
Sustainable energy solutions for hospitals
Hospitals need sustainable energy solutions, not only to reduce operating costs but also to minimize environmental impact and attain energy security. Harnessing renewable energies like solar and wind, the implementation of microgrid systems for local management of energy, and the examination of case studies of hospitals using these solutions are crucial aspects of modern hospital infrastructure.
Incorporation of renewable energy sources: solar and wind energy
Integration of solar and wind renewable energy sources into hospital power supply systems can be beneficial to reduce dependence on grid power, save on electricity bills, and reduce carbon emissions. The power produced from the renewable sources can be determined mathematically.
The amount of power generated by a solar panel is dependent on several factors such as solar irradiance, the efficiency of the solar cells, and the area of the panels. The total power generated by the solar system \(\:{P}_{solar}\left(t\right)\)at time \(\:t\) can be written as:
$$\:{P}_{solar}\left(t\right)=A.I\left(t\right).\eta\:$$
(9)
where \(\:A\) is the area of the solar panels in square meters (m2). \(\:I\) is the solar irradiance at time \(\:t\) (measured in W/m2). \(\:\eta\:\) is the efficiency of the solar panels.
The energy flow and balance in the rooftop solar PV system integrated into the healthcare infrastructure can be expressed through the following energy equation:
$$\:{E}_{p}={E}_{f}+{E}_{Net}$$
(10)
where \(\:{E}_{p}\) is Energy produced by the solar panel (DC energy), \(\:{E}_{f}\)Energy consumed by the facility’s internal load (converted to AC), \(\:{E}_{Net}\) Surplus energy exported to the utility grid via the net meter.
Figure 2 illustrates the integration of a rooftop solar photovoltaic (PV) system into a healthcare facility’s electrical network. Solar panels mounted on the rooftop capture solar energy and convert it into direct current (DC) electricity, represented as \(\:{E}_{P}\), which flows into the DC bus. This energy is then converted into alternating current (AC) by a converter to supply power to hospital loads such as lighting, life-support systems, and other critical equipment. The generated electricity is first used to meet the internal energy demand \(\:{E}_{I}\), and any excess energy \(\:{E}_{Net}\) is exported to the utility grid through a medium-voltage (MV) net meter. The system connects to the public grid via a distribution transformer that links the facility’s low-voltage (LV) network to the MV network. This setup enhances energy self-sufficiency, reduces dependency on the grid, and improves overall energy efficiency and sustainability in healthcare infrastructure.
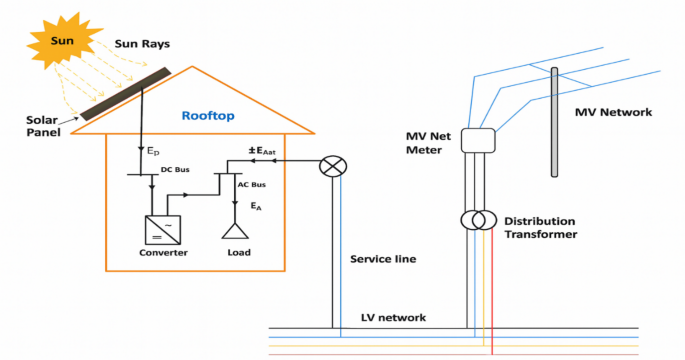
Integration of a rooftop solar photovoltaic (PV) system into a healthcare facility.
The power generated by a wind turbine is influenced by the wind speed and the characteristics of the turbine. The total power generated by a wind turbine \(\:{P}_{wind}\left(t\right)\) can be expressed by the following equation:
$$\:{P}_{wind}\left(t\right)=\frac{1}{2}\:.\rho\:\:.\:{A}_{wind}.{C}_{p}.{v}^{3}\left(t\right)$$
(11)
where \(\:\rho\:\) is the air density (kg/m³). \(\:{A}_{wind}\) is the swept area of the turbine blades (m2). \(\:{C}_{p}\) is the power coefficient of the turbine (typically between 0.25 and 0.45). \(\:{v}^{3}\left(t\right)\) is the wind speed at time \(\:t\) (m/s).
Both solar and wind energy sources can be integrated into the hospital’s grid using power converters and storage systems, such as batteries or flywheels, to ensure continuous power supply during periods of low generation.
Implementation of microgrid systems for localized energy management
Microgrid systems provide localized energy management and control, which can improve energy resilience, reduce reliance on the main grid, and optimize the integration of renewable sources. A hospital microgrid typically includes distributed energy sources (solar, wind, and backup generators), energy storage systems, and a local grid controller.
The total energy demand of the hospital \(\:{P}_{demand}\left(t\right)\) is met by a combination of grid power \(\:{P}_{grid}\left(t\right)\), renewable energy \(\:{P}_{renewable}\left(t\right)\), and stored energy from batteries \(\:{P}_{battery}\left(t\right)\). The microgrid’s energy balance equation can be expressed as:
$$\:{P}_{demand}\left(t\right)={P}_{grid}\left(t\right)+{P}_{renewable}\left(t\right)+{P}_{battery}\left(t\right)$$
(12)
where \(\:{P}_{demand}\left(t\right)\) is the total energy demand at time \(\:t\). \(\:{P}_{grid}\left(t\right)\) is the energy drawn from the main grid. \(\:{P}_{renewable}\left(t\right)\) is the energy supplied by renewable sources (solar and wind). \(\:{P}_{battery}\left(t\right)\) is the energy supplied by battery storage systems.
To ensure that the battery system is charged efficiently, the energy balance equation for battery charging \(\:{P}_{battery}\left(t\right)\:\)can be written as:
$$\:{P}_{battery}\left(t\right)={P}_{charging}\left(t\right)-{P}_{discharging}\left(t\right)$$
(13)
where \(\:{P}_{charging}\left(t\right)\) is the rate at which the battery is charged. \(\:{P}_{discharging}\left(t\right)\) is the rate at which the battery discharges to meet the hospital’s demand.
Microgrid controllers use optimization algorithms to manage the distribution of power, considering factors such as cost, reliability, and environmental impact. The controller aims to minimize the total operating cost \(\:{C}_{total}\), which is the sum of costs associated with grid power, renewable energy generation, and battery usage:
$$\:{C}_{total}={C}_{grid}+{C}_{renewable}+{C}_{battery}$$
(14)
where \(\:{C}_{total}={P}_{grid}\left(t\right).\:{c}_{grid}\:\)is the cost of energy drawn from the grid. \(\:{C}_{renewable}={P}_{renewable}\left(t\right){.c}_{renewable}\) is the cost of energy from renewable sources. \(\:{C}_{battery}={P}_{battery}\left(t\right).{c}_{battery}\) is the cost of energy from battery storage.
The goal of the microgrid controller is to minimize \(\:{C}_{total}\) while meeting the hospital’s demand:
$$\:min{C}_{total}\:subject\:to\:{P}_{demand}\left(t\right)={P}_{grid}\left(t\right)+{P}_{renewable}\left(t\right)+{P}_{battery}\left(t\right)$$
(15)
Hospital load uncertainty modeling
Hospital load uncertainty arises due to unpredictable variations in patient occupancy, emergency procedures, medical equipment operation schedules, and ambient climate conditions38. Unlike conventional commercial buildings, hospital energy demand cannot be fully predicted using static profiles because emergency departments, operating theatres, and intensive care units exhibit stochastic load behaviors influenced by patient inflow and diagnostic activities.
To address this challenge, an uncertainty-aware load model was developed using probabilistic and machine learning approaches. The model represents hospital demand \(\:{P}_{t}\)as a combination of deterministic baseline load \(\:{P}_{b}\)and stochastic fluctuation \(\:{\epsilon\:}_{t}\):
$$\:{P}_{t}={P}_{b}+{\epsilon\:}_{t}$$
(16)
where \(\:{\epsilon\:}_{t}\sim\mathcal{\:}\mathcal{N}\left(0,\:{\sigma\:}^{2}\right)\) represents random deviations in load caused by operational or environmental factors. The variance \(\:{\sigma\:}^{2}\)was estimated from historical IoT-based load data collected across intensive care units, operating theatres, and diagnostic departments.
The reinforcement learning (RL) controller dynamically updated resource dispatch policies in real time to mitigate risk during unexpected load spikes, ensuring uninterrupted supply to critical areas39. This uncertainty-aware modeling approach strengthens the reliability of the proposed AI-driven energy management system, enabling hospitals to maintain power stability and efficiency even during extreme or unforeseen operational conditions such as pandemics, equipment failures, or emergency surges.
System configuration and load composition
The hospital energy management framework was modeled based on actual operational zones, equipment inventories, and departmental load characteristics. Each department exhibits distinct consumption behavior depending on its function, occupancy pattern, and HVAC dependency.
Table 6 presents the detailed breakdown of electrical appliances, their rated capacities, operational durations, and corresponding daily energy consumption across key hospital departments. This quantitative dataset forms the foundational input for the load forecasting and reinforcement learning optimization modules.
As shown in Table 6, the ICU and ward zones collectively account for nearly half of the hospital’s total daily energy consumption, primarily due to continuous operation of life-support systems and HVAC requirements. Radiology and operating rooms also demonstrate high specific energy intensity owing to diagnostic and sterilization loads. These appliance-level data were used to train the LSTM forecasting model and parameterize the AI-driven optimization framework described in Sect. 4.
HVAC energy efficiency strategy
HVAC systems represent the dominant share of hospital energy consumption, accounting for approximately 38–40% of total daily load. To enhance operational efficiency without compromising patient comfort or indoor air quality, an AI-assisted control framework was developed to dynamically regulate HVAC operation according to occupancy, environmental conditions, and renewable-energy availability. HVAC energy reduction is achieved through adaptive set-point control, occupancy-based variable-air-volume (VAV) scheduling, and supervisory AI coordination with renewable generation.
In the adaptive control layer, predictive thermal-comfort models adjust temperature set-points within the comfort range of 22–25 °C based on real-time occupancy and outdoor conditions. This proactive regulation minimizes compressor cycling and maintains compliance with ASHRAE 55-2021 comfort standards40. The occupancy-based control mechanism modulates air-supply volume to each zone according to activity intensity, reducing airflow by up to 40% in unoccupied areas and thereby lowering chiller and fan power consumption. At the supervisory level, the AI controller aligns HVAC operation with solar PV and wind energy availability by initiating pre-cooling or pre-heating during peak renewable generation periods. This strategy reduces grid dependency and facilitates thermal energy storage within the building envelope.
To validate HVAC energy modeling and ensure realistic load distribution, the hospital building was divided into six primary thermal zones according to function, floor area, and occupancy patterns. Table 7 summarizes the zoning configuration and operational characteristics used in the simulation. Critical-care and ward zones maintain continuous conditioning to support clinical stability, while diagnostic and laboratory areas follow daytime operation cycles. Administrative and support spaces are scheduled for office-hour cooling only, with reduced ventilation during non-occupied hours. This zoning structure provides accurate thermal-load estimation and validates the distribution of HVAC power demand across the simulated model.
link